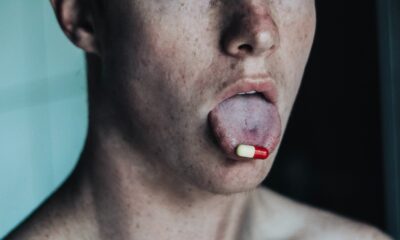
The University of California, Davis has launched the Institute for Psychedelics and Neurotherapeutics to advance basic knowledge about the mechanisms of psychedelics.
The Institute for Psychedelics and Neurotherapeutics will work to translate this knowledge into safe and effective treatments for diseases such as depression, post-traumatic stress disorder (PTSD), addiction, Alzheimer’s disease and Parkinson’s disease, among others.
Bringing together scientists across a range of disciplines, the Institute will partner with the pharmaceutical industry to ensure that key discoveries lead to new medicines for patients.
Associate professor in the Department of Chemistry and the Department of Biochemistry and Molecular Medicine at UC Davis, David E. Olson, will be the founding director and John A. Gray, associate professor in the Department of Neurology, will serve as associate director.
In 2018, Olson and Gray published an influential study in Cell Reports demonstrating that psychedelics promote neuroplasticity — the growth of new neurons and formation of neural connections.
Olson commented: “Psychedelics have a unique ability to produce long-lasting changes in the brain that are relevant to treating numerous conditions.
“If we can harness those beneficial properties while engineering molecules that are safer and more scalable, we can help a lot of people.”
Gray added: “Neuronal atrophy is a key factor underlying many diseases, and the ability of psychedelics to promote the growth of neurons and new connections in the brain could have broad therapeutic implications.”
A historic investment
The UC Davis institute will be funded in part by a contribution of approximately USD$5 million from the deans of the College of Letters and Science and the School of Medicine, the Vice Chancellor for Research and the Provost’s office.
The University highlights that, while other psychedelic science centres have been formed across the country with gifts from philanthropists, the UC Davis institute is notable for also being supported by substantial university funds.
Dean of the College of Letters and Science, overseeing the new institute, Estella Atekwana, commented: “We wanted to put our money where our mouth is and demonstrate our commitment to this space.
“UC Davis has been leading the development of new medicines based on psychedelic research, and together with philanthropists, granting agencies and industrial partners, I’m confident that we can produce major benefits for society.”
Philanthropic donations as well as grants and sponsored research agreements from the federal government, private foundations and industry partners will also support the mission of the institute.
Leveraging strengths in chemistry, neuroscience and medicine
The institute will leverage the expertise in the neuroscience community at UC Davis, which includes nearly 300 faculty members in centres, institutes and departments across the Davis and Sacramento campuses. Researchers will be able to work on every aspect of psychedelic science, from molecules and cells through to human clinical trials.
Susan Murin, dean of the School of Medicine who partnered with Atekwana to support the new institute, commented: “Combining the considerable expertise of UC Davis’ pioneering basic research teams, world-class neuroscientists and our nationally recognised medical centre is a formula for success that we trust will result in groundbreaking discoveries that will help patients regionally and worldwide.”
The Institute for Psychedelics and Neurotherapeutics was specifically designed to facilitate collaborations across campus, such as that between Olson and Lin Tian, a professor in the Department of Biochemistry and Molecular Medicine. In 2021, their publication in Cell was voted the #2 biomedical research discovery of the year by STAT Madness.
A unique feature of the UC Davis institute will be its focus on chemistry and the development of novel neurotherapeutics.
“Psychedelics have a lot of therapeutic potential, but we can do better,” said Olson.
Bridging the Valley of Death between academia and industry
The University emphasises that major challenges exist in translating academic discoveries and promising lead compounds into drug candidates for clinical use. To bridge this gap, it has stated that the Institute aims to spin out companies and build strong collaborations with pharmaceutical partners through licensing and sponsored research agreements.
Delix Therapeutics, a company co-founded by Olson, has licensed UC Davis technology and supported several cutting-edge basic research projects on campus related to psychoplastogens and neuroplasticity. Recently, Delix was named a top academic spinout company by Nature Biotechnology and C&E News, and in 2021, was named one of the Fierce 15 by Fierce biotech.
“Our relationship with UC Davis has been very synergistic, and we are excited to continue that partnership,” said Mark Rus, the CEO of Delix. “Getting the brightest and most creative minds from academia and industry to work together is our best chance to solve many of the grand challenges facing society today.”

 Opinion2 years ago
Opinion2 years ago
 Insight3 years ago
Insight3 years ago
 Medicinal2 years ago
Medicinal2 years ago
 Research2 years ago
Research2 years ago
 Medicinal2 years ago
Medicinal2 years ago
 Markets & Industry1 year ago
Markets & Industry1 year ago
 News3 years ago
News3 years ago
 Research2 years ago
Research2 years ago